By: Julia K. Böhm, Helge Güting, Sophie Thorn, Nadine Schäfer, Victoria Rambach, Herbert Schöchl, Oliver Grottke, Rolf Rossaint, Simon Stanworth, Nicola Curry, Rolf Lefering, Marc Maegele & CENTER-TBI Participants and Investigators
First Online: 11 December 2020
Background
Trauma-induced coagulopathy in patients with traumatic brain injury (TBI) is associated with high rates of complications, unfavourable outcomes and mortality. The mechanism of the development of TBI-associated coagulopathy is poorly understood.
Methods
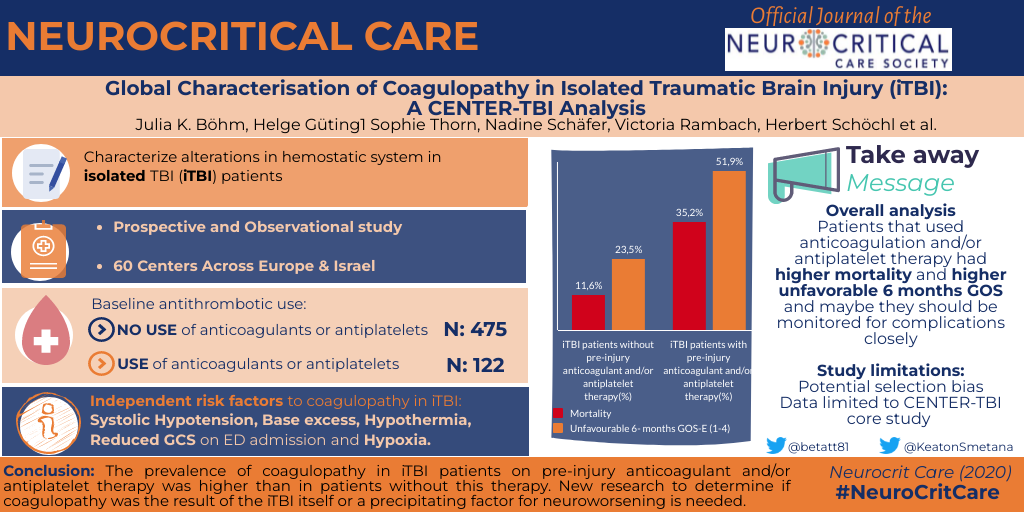
This analysis, embedded in the prospective, multi-centred, observational Collaborative European NeuroTrauma Effectiveness Research in Traumatic Brain Injury (CENTER-TBI) study, aimed to characterise the coagulopathy of TBI. Emphasis was placed on the acute phase following TBI, primary on subgroups of patients with abnormal coagulation profile within 4 h of admission, and the impact of pre-injury anticoagulant and/or antiplatelet therapy. In order to minimise confounding factors, patients with isolated TBI (iTBI) (n = 598) were selected for this analysis.
Results
Haemostatic disorders were observed in approximately 20% of iTBI patients. In a subgroup analysis, patients with pre-injury anticoagulant and/or antiplatelet therapy had a twice exacerbated coagulation profile as likely as those without premedication. This was in turn associated with increased rates of mortality and unfavourable outcome post-injury. A multivariate analysis of iTBI patients without pre-injury anticoagulant therapy identified several independent risk factors for coagulopathy which were present at hospital admission. Glasgow Coma Scale (GCS) less than or equal to 8, base excess (BE) less than or equal to − 6, hypothermia and hypotension increased risk significantly.
Conclusion
Consideration of these factors enables early prediction and risk stratification of acute coagulopathy after TBI, thus guiding clinical management.
Read full article here.